Genetic Testing in Psychiatry: High Hopes vs. Hard Science
It’s one of the most common questions I hear in my office: "Can’t we just do a genetic test to see which medication will work for me?"
It sounds like a dream scenario. Instead of the "trial and error" process that often accompanies psychiatric treatment, we’d simply take a cheek swab, run a report, and find your perfect biological match.
However, as much as I wish I could offer that shortcut, the reality of pharmacogenomic (PGx) testing today is much more complicated. While these tests are marketed as a way to "take the guesswork out of mental health," their actual clinical utility remains quite limited.
Patients can understandably become frustrated during the “trial-and-error” process of finding the right medication. While there are significant differences between medications for ADHD, depression, and many other conditions, there is not a single test that can accurately map those differences onto an individual human brain to predict success.
The Big Misconception: Effectiveness vs. Metabolism
The most important thing to understand is what these tests can and cannot tell us.
What they CANNOT do: Predict which medication will actually make you feel better. Currently, we do not have the technology to look at your DNA and accurately say, "Drug A will cure your depression, but Drug B will not."
What they CAN do: Identify how your body processes certain chemicals. This is known as pharmacokinetics.
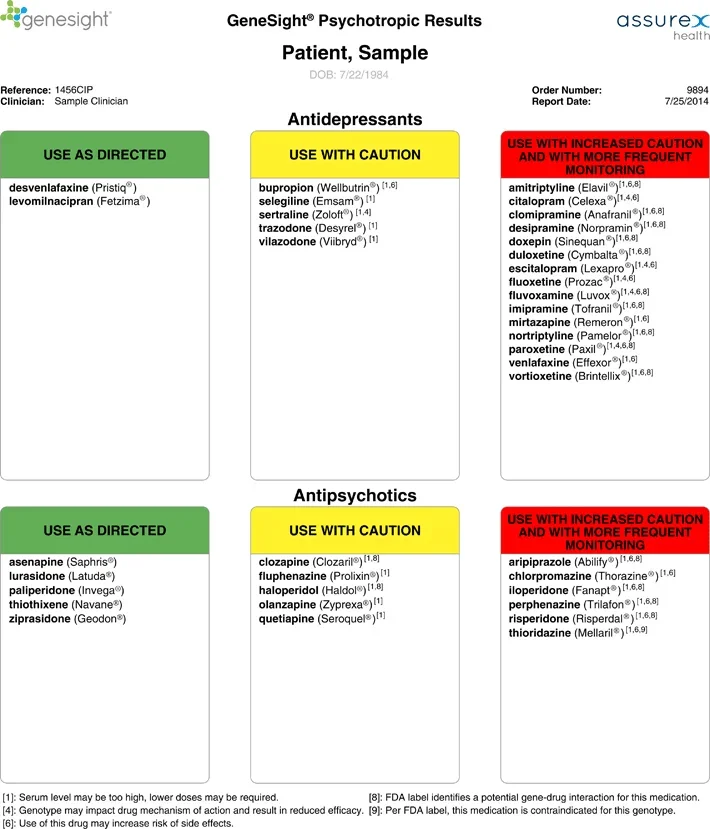
This is the typical look of genetic testing results. Patients are often scared when they find out they are taking something marked “Yellow” or “Red,” but in reality, these medications can still be used with careful monitoring.
When the Tests Are (Somewhat) Useful
The one area where genetic testing provides real value is in identifying metabolizer status. Your liver uses specific enzymes (like the CYP450 system) to break down medications.
A genetic test might reveal that you are:
A Rapid Metabolizer: Your body clears the drug so quickly that standard doses never reach a therapeutic level in your bloodstream. In this case, we might safely use a higher-than-normal dose.
A Poor (Slow) Metabolizer: The drug lingers in your system too long, increasing the risk of toxicity or intense side effects. For these patients, we "go low and slow" with dosing to ensure safety.
The Bottom Line: Cost vs. Utility
Despite the slick color-coded reports (often using "Red, Yellow, and Green" categories), these tests are often expensive and, for the vast majority of patients, offer no real clinical value beyond what we can learn through careful observation and standard prescribing practices.
Key Takeaway: A "Green" result on a genetic report does not mean a drug will work for you; it simply means your body is likely to break it down at a normal rate. You can still have zero response to a "Green" drug or a fantastic response to a "Yellow" or “Red” one.
How We Move Forward
Psychiatry is still a deeply human science. While we wait for the technology to catch up to the marketing, the most effective "test" remains a thorough clinical evaluation, a look at your family history (which is a powerful, free genetic indicator!), and a collaborative relationship between doctor and patient.
If you’ve been frustrated by the process of finding the right medication, know that it isn't because we’re missing a simple test—it’s because your brain is one of the most complex structures in the world. Neuroscience is a constantly evolving field, one without simple mechanisms and algorithms to follow. Evidence-based care and human understanding remain much more potent tools than highly marketed genetic testing kits.
About the Author: Thomas Scary, MD
Board-Certified Psychiatrist
Dr. Thomas Scary is a medical doctor specializing in comprehensive psychiatric care. With offices in Center City Philadelphia and Ambler, PA, his practice focuses on evidence-based treatment plans that integrate medical expertise with a patient-centered approach. Dr. Scary is dedicated to providing transparent, accessible mental health education to help patients make informed decisions about their care.
Medical Disclaimer: This content is for informational purposes only and does not constitute medical advice. Although AI tools are used to assist in formatting and research, every article is personally reviewed, edited, and verified for clinical accuracy by Thomas Scary, MD.
Visit Dr. Scary in Person
255 S. 17th St. Suite 2902 Philadelphia, PA 19103
Ideal for professionals working in Rittenhouse or Old City.
748 N. Bethlehem Pike Suite 202 Lower Gwynedd, PA 19002
Conveniently located for Bala Cynwyd and Main Line families.